Chapter 14
Unilateral Hyperlucent Hemithorax
Learning Objectives
- Recognize a unilateral hyperlucent hemithorax on a chest radiograph or computed tomography (CT).
- Describe the common causes of a unilateral hyperlucent hemithorax on a chest radiograph or CT.
- List an appropriate differential diagnosis when a hyperlucent hemithorax is seen on a chest radiograph or CT and suggest a specific diagnosis when certain associated findings are seen (e.g., absence of a breast after mastectomy, absence of a pectoralis muscle in Poland syndrome, unilateral or asymmetric bullous disease/emphysema, or air trapping on exhalation imaging in a patient with Swyer-James syndrome or an endobronchial foreign body).
The most common chest radiographic causes of a
unilateral hyperlucent hemithorax do not reflect an intrinsic
abnormality of the lung itself. Improper patient positioning is the
most common cause. A slight degree of patient rotation will result in
disparity in overall lung opacity on the posteroanterior (PA) chest
radiograph. By the same mechanism, scoliosis, if severe, may cause
asymmetry of lung density. Mastectomy results in asymmetry of soft
tissues overlying the lungs and relative radiolucency on the side of
breast removal (Fig. 14-1). This common cause
of unilateral hyperlucent hemithorax is easily overlooked unless the
observer is methodical in always evaluating soft tissues on a chest
radiograph. Absence of the sternocleidomastoid muscle results in
hyperlucency in the upper hemithorax (Fig. 14-2). Absence of the pectoralis muscle also results in hyperlucency of the ipsilateral hemithorax (Fig. 14-3 and 14-4). When associated with ipsilateral syndactyly, brachydactyly, and rib anomalies, the condition is called Poland syndrome.
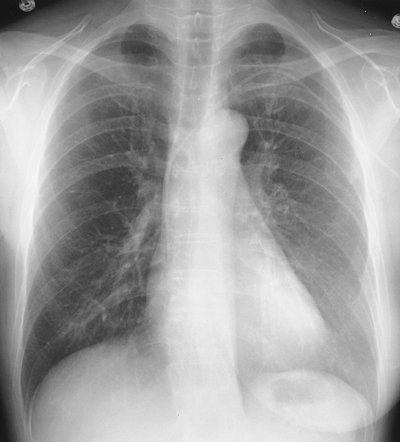 |
FIGURE 14-1. Mastectomy.
PA chest radiograph of a woman after right mastectomy for breast
cancer. Note the presence of a breast shadow on the left and the
absence on the right; as a result, the right lung appears relatively
hyperlucent compared with the left. |
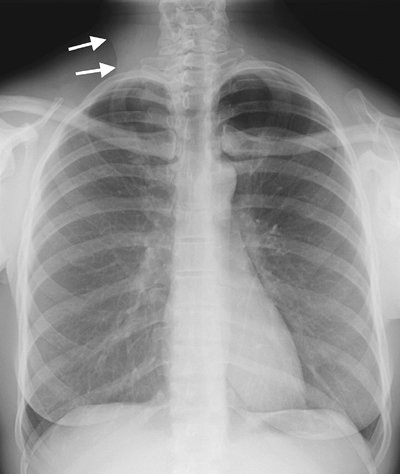 |
FIGURE 14-2. Absence of sternocleidomastoid muscle.
PA chest radiograph of a 47-year-old woman with thyroid carcinoma who
underwent left radical neck dissection shows hyperlucency of the left
upper hemithorax. Note a normal sternocleidomastoid muscle shadow on
the right (arrows) and absence of the shadow on the left. |
P.239
 |
FIGURE 14-3. Absence of pectoralis muscle.
PA chest radiograph shows relative hyperlucency of the left hemithorax
because of the absence of left pectoralis muscle. Note the normal
pectoralis muscle shadow on the right (solid arrow) and abnormal elevation of the skin fold on the left (dashed arrow). |
A large pneumothorax results in hyperlucency of the
ipsilateral hemithorax and can be recognized by observing displacement
of the visceral pleural line, absence of lung markings distal to the
displaced pleural line, and contralateral shift of the mediastinum (Fig. 14-5).
Patients who have had pulmonary resections or who have lobar
atelectasis may also show lucency of the residual aerated lung in the
involved hemithorax because of compensatory hyperexpansion. A common
cause of hyperlucent hemithorax in some hospitals is unilateral lung
transplantation for pulmonary emphysema, where the native emphysematous
lung is radiolucent relative to the lung transplant, which receives the
bulk of the pulmonary perfusion (Fig. 14-6). In
some cases of hyperlucent hemithorax, the lucent side is normal and the
opposite side is abnormally radiopaque. Diffuse pleural thickening on
the more opaque side or pleural fluid layering posteriorly on a supine
radiograph are frequent causes.
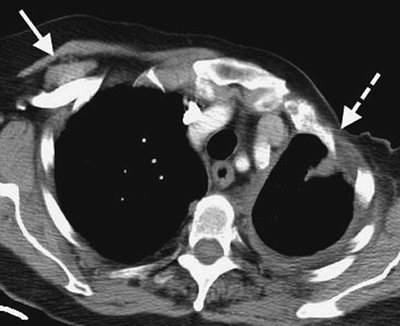 |
FIGURE 14-4. Absence of pectoralis muscles.
Computed tomography (CT) of a woman who underwent left radical
mastectomy for breast cancer shows pectoral muscles on the right (solid arrow) and absence of pectoral muscles on the left (dashed arrow). |
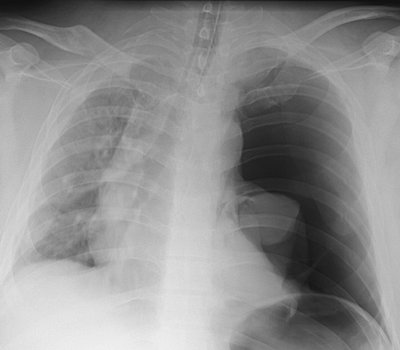 |
FIGURE 14-5. Tension pneumothorax.
Anteroposterior supine chest radiograph of a 35-year-old man involved
in a motor vehicle crash shows a large left pneumothorax, collapse of
the left lung, and mediastinal shift to the right. The left hemithorax
is hyperlucent compared with the right. |
The origins of true unilateral hyperlucent lung will be
the focus of this chapter. After faulty radiologic technique and chest
wall defects are excluded as possible sources, the causes of unilateral
hyperlucent lung can be categorized into those primarily related to
airway obstruction and those primarily related to decreased pulmonary
blood flow (Table 14-1).
 |
FIGURE 14-6. Left lung transplant.
PA chest radiograph of a 62-year-old woman with a left lung transplant
shows a hyperlucent right lung. The native right emphysematous lung is
hyperlucent and hyperexpanded, causing mediastinal shift to the left. |
P.240
TABLE 14-1 CAUSES OF UNILATERAL HYPERLUCENT HEMITHORAX | |
|---|---|
|
Airway Obstruction As a Cause of Unilateral Hyperlucent Lung
The hallmark of airway obstruction on chest radiographs
is the finding of air trapping. An exhalation-phase chest radiograph
will show whether air trapping is present; this is manifested as
failure of the lung to decrease in volume and failure of the lung to
increase in opacity on exhalation compared with inhalation. In some
cases, the mediastinum shifts to the side that is not trapping air on
exhalational views. Air trapping occurs when an endobronchial lesion,
usually a foreign body in a large airway, causes a check-valve type of
obstruction. The foreign body does not completely obstruct the bronchus
in which it is lodged. During inhalation, the bronchial diameter
normally increases, allowing air to pass around the foreign body and
enter the lung distal to the obstruction. During exhalation, the
bronchial diameter normally decreases, and the air is trapped within
the lung distal to the obstruction. This allows a foreign body that
does not completely obstruct a bronchus during inhalation to do so
during exhalation. As a result, the lung, lobe, or segment distal to
the foreign body becomes increasingly distended until the pressure
within it prevents more air from entering. In children, this type of
check-valve obstruction usually results from the aspiration of food,
commonly a peanut, or a toy or coin. In adults, this type of
obstruction can result from aspiration of foreign bodies but also, more
important, from an endobronchial tumor (Fig. 14-7). Extrinsic masses, such as
enlarged nodes or an enlarged heart, can obstruct a bronchus in a similar fashion.
P.241
enlarged nodes or an enlarged heart, can obstruct a bronchus in a similar fashion.
 |
FIGURE 14-7. Carcinoid tumor. A:
PA inspiratory chest radiograph of a 24-year-old woman with a prolonged
history of wheezing, shortness of breath, cough, and recurrent
pneumonia appears normal. The patient was treated for asthma with no
relief in symptoms. B: PA exhalational view shows air trapping in the left hyperlucent lung and mediastinal shift to the right. C: CT shows a mass (arrow)
in the left main bronchus. This mass results in a ball-valve
obstruction, where air enters the lung during inhalation but can't exit
the lung during exhalation. Note that the left lung is hyperlucent
relative to the right lung as a result of air trapping. |
Obliterative bronchiolitis is a syndrome of airflow limitation caused by bronchiolar and peribronchiolar inflammation and fibrosis, as was discussed in Chapter 13.
In adults, it is most often idiopathic in etiology, but is also
associated with lung and bone marrow transplantation as well as a
variety of other insults to the lung. The Swyer-James, or MacLeod, syndrome is a form of obliterative bronchiolitis that occurs following an insult to the developing lung (1).
In this syndrome, unlike in large central airway obstruction, small
bronchi and bronchioles are affected, and the lung served by abnormal
airways remains inflated by collateral air drift. By definition, the
airway disease as assessed by the chest radiograph is predominantly
unilateral, giving rise to the key finding of unilateral hyperlucent
lung. In practice, obliterative bronchiolitis is often bilateral and
patchy. The injury to the immature lung, which occurs during the first
8 years of life, commonly follows a viral infection. Bronchi and
bronchioles from the fourth generation to the terminal bronchioles have
submucosal fibrosis, which causes luminal irregularity and occlusion.
Pulmonary tissue is hypoplastic, including the pulmonary artery and its
branches, which are reduced in both size and number. Lung distal to
diseased airways is hyperinflated and supplied by collateral air drift.
Sometimes panacinar emphysematous changes are present. Patients are
typically asymptomatic, often presenting as adults with an incidental
abnormal chest radiograph.
Chest radiographs show unilateral hyperlucency because of reduced lung perfusion and air trapping (Fig. 14-8).
The size and number of vessels in the middle and peripheral lung are
reduced on the affected side. The hilum of the involved lung is small,
but lung volumes are normal or only slightly decreased. Ipsilateral air
trapping on exhalational chest radiography is a key finding of the
condition. The air trapping can also be demonstrated on nuclear
medicine ventilation studies or paired inhalation/exhalation computed
tomography (CT).
The CT findings of Swyer-James syndrome include a
patchwork of local low-density and hypovascular areas interspersed with
lung of normal density (2). Air trapping can be
confirmed on exhalation. Other changes that can be seen on CT include
bronchiectasis, bronchiolectasis, atelectasis, and focal scarring (see Fig. 13-26) (3).
Pulmonary emphysema is a
pathologic diagnosis that is defined as a condition of the lung
characterized by abnormal permanent enlargement of airspaces distal to
the terminal bronchiole and accompanied by the destruction of their
walls and without obvious fibrosis. Although emphysema is usually a
diffuse, bilateral process, it can on occasion be asymmetric, with one
lung more severely involved than the other. This marked asymmetry in
involvement can result in the more severely involved lung appearing
hyperlucent compared with the opposite lung (Fig. 14-9). Emphysema is discussed in more detail in Chapter 13.
 |
FIGURE 14-8. Swyer-James syndrome.
PA chest radiograph of a 12-year-old boy shows hyperlucency of the
abnormal left lung. The vessels on the left are diminutive, the hilum
is small, and lung volume is slightly decreased. |
 |
FIGURE 14-9. Asymmetric pulmonary emphysema. A: PA chest radiograph of a 69-year-old woman with emphysema shows hyperlucency of the right lung. B:
CT shows the cause of the hyperlucency to be emphysema that more
severely involves the right lung compared with the left lung. The
vessels in the right lung are diminutive compared with those on the
left. |
Congenital lobar emphysema (CLE) usually manifests in the neonatal period, but in some cases the presentation is delayed
until after the first month of life; it can also present in adulthood. Aplasia, hypoplasia, or dysplasia of bronchial supporting structures is postulated as the primary cause of CLE (4). The chest radiographic appearance of CLE is hyperexpansion of an isolated lobe in one lung, usually an upper or middle lobe. The expanded lobe may cause compressive atelectasis of the rest of the lung. Its appearance on chest radiography or CT can be similar to that of obliterative bronchiolitis.
P.242
until after the first month of life; it can also present in adulthood. Aplasia, hypoplasia, or dysplasia of bronchial supporting structures is postulated as the primary cause of CLE (4). The chest radiographic appearance of CLE is hyperexpansion of an isolated lobe in one lung, usually an upper or middle lobe. The expanded lobe may cause compressive atelectasis of the rest of the lung. Its appearance on chest radiography or CT can be similar to that of obliterative bronchiolitis.
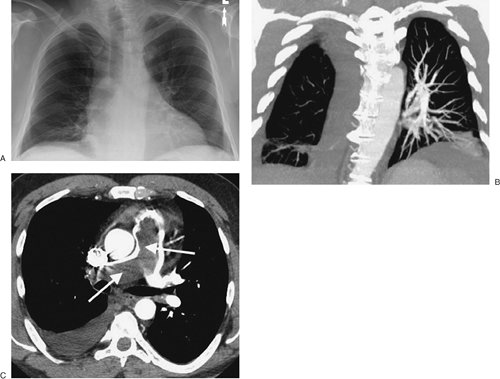 |
FIGURE 14-10. Pulmonary emboli. A:
PA chest radiograph of a man with a lower-extremity soft tissue
sarcoma, embolizing to the pulmonary arteries, shows a hyperlucent
right lung. B: Coronal reformatted CT shows markedly decreased perfusion to the right lung. C: Axial CT shows low-attenuation filling defect throughout the main and right pulmonary arteries (arrows). |
Pulmonary Vascular Causes of Unilateral Hyperlucent Lung
Pulmonary vascular conditions may result in a
hyperlucent lung on chest radiography that is indistinguishable from
the lucency associated with airway obstruction. However, in primary vascular conditions, air trapping is generally not as severe as with airway obstruction.
One of the chest radiographic signs of pulmonary
embolism is oligemia of the lung beyond the occluded vessel (Westermark
sign). A large unilateral embolus, whether bland, septic, or
neoplastic, can result in a unilateral hyperlucent lung (Fig. 14-10).
When seen, the Westermark sign can be very helpful in suggesting
further workup for pulmonary embolism in the appropriate patient
population; however, this sign is not commonly seen. A more detailed
discussion of radiographic and CT findings of pulmonary embolism is
included in Chapter 17.
Unilateral absence or hypoplasia of a lung or a lobe is
a congenital abnormality that, surprisingly, may cause few clinical
problems when not accompanied by other congenital abnormalities. The
chest radiographic findings are those of absent or decreased aeration
of the affected side, signs of volume loss, and compensatory
hyperaeration of the opposite lung. The decreased perfusion to the
affected lung contributes to its relative hyperlucency. Radiographs,
and especially CT, show the diminution or absence of a pulmonary
artery. Fibrosing mediastinitis, when associated with encasement of a
pulmonary artery by fibrous tissue, can produce a similar appearance.
In this case, however, CT will show the abnormal fibrous tissue
infiltrating the mediastinum and encasing the bronchi and vessels.
References
1. Reid L, Simon G. Unilateral lung transradiancy. Thorax. 1962;17:230–239.
2. Moore ADA, Godwin JD, Dietrich PA, et al. Swyer-James syndrome: CT findings in eight patients. AJR Am J Roentgenol. 1992;158:1211–1215.
3. Marti-Bonmati L, Perales FR, Catala F, et al. CT findings in Swyer-James syndrome. Radiology. 1989;172:477–480.
4. Stovin PGI. Congenital lobar emphysema. Thorax. 1959;14:254–261.